Bone grafting is a common dental procedure used to rebuild parts of the jaw that have lost bone. This often happens after tooth loss, gum disease, injury, or infection.
When the jawbone becomes too thin, it may no longer support a dental implant or even nearby teeth. Bone grafting teeth in these situations helps rebuild lost structure, restore stability, and protect long‑term oral function. This can affect chewing, appearance, and overall oral stability.
Bone grafting involves placing special material in the affected area to encourage new bone growth. Over time, this restores strength and volume to the jaw, making future dental treatments possible.
At Burnaby Dentist & Orthodontist, we use digital 3D imaging and CBCT scans to assess jawbone health and determine when grafting is the right next step. This allows us to plan treatments that restore bone structure, protect your facial profile, and prepare your mouth for long-term stability.
At a Glance:
Dental bone grafting restores lost jawbone caused by missing teeth, gum disease, or trauma. It helps improve chewing, protect facial structure, and support future dental implants. Healing is manageable with proper care, and your dentist will choose the right technique based on your needs.
Why Jaw Volume Matters
Your jawbone isn’t just there to hold your teeth. It supports your facial shape, your bite, and your long-term oral health. When bone volume is lost, it affects more than just one area.
Here’s how reduced jawbone density can impact your dental future:
- Implant Stability: Dental implants need a solid base to stay secure. Without enough bone height or width, integration becomes difficult.
- Facial Appearance: Bone loss can cause the skin around your mouth to sag, leading to a prematurely aged or hollow look.
- Neighbouring Teeth and Gums: As bone weakens, nearby teeth lose support, increasing the risk of shifting and gum recession.
Quick Wins of Early Grafting
Acting early simplifies treatment and helps maintain a healthy foundation for future restorative dentistry. Early bone grafting offers:
- Preserves ridge shape for future restorative treatments
- Keeps options open for dental implants and stable bite correction
- Supports facial contours and prevents early signs of collapse
Types of Dental Bone Grafts and When They’re Used
Dental bone grafts vary not only in material but also in how and when they’re placed. At Burnaby Dentist & Orthodontist, we personalize your treatment using digital imaging and CBCT scans to choose the most effective graft type for your needs.
Graft Materials Explained: What Your Bone Graft May Be Made Of
Each graft material has distinct advantages based on healing goals, surgical complexity, and your medical background. Here’s how they compare:
1. Autograft (Your Own Bone)
Autografts are taken from another part of your body, often the chin, jaw, or hip. Since this bone is living tissue from your own system, it’s fully compatible and naturally supports healing.
Autografts are considered the “gold standard” because they promote bone growth in three ways: they provide a structure, stimulate new cell formation, and bring live bone-forming cells to the area.
However, this approach does require a second surgical site, which can mean more recovery time.
2. Allograft (Human Donor Bone)
Allografts use bone from a screened human donor, typically processed and sterilized by a bone bank. These grafts support healing without needing to harvest bone from your own body.
They contain growth proteins that encourage your bone to regenerate over time. While they don’t offer live cells like autografts, they’re widely used and effective, especially in implant preparation and periodontal treatment.
3. Xenograft (Animal Bone)
Xenografts are derived from animal sources, usually bovine (cow). They act as a scaffold for your natural bone to grow into.
Because xenografts break down more slowly than other types, they’re ideal when long-term support is needed, such as preserving bone height after a tooth extraction.
However, they typically require a longer healing time before implant placement.
4. Alloplast (Synthetic Graft)
Alloplasts are made from synthetic materials like calcium phosphate or hydroxyapatite. They don’t contain any biological tissue, so there’s no risk of disease transfer or immune response.
These grafts offer structural support and are often used in smaller bone repairs. While they don’t stimulate growth as powerfully as natural grafts, they can be a safe and effective choice depending on your needs.
Common Grafting Techniques: When and Where They’re Used
In addition to material, the timing and location of your graft affects healing and future implant planning. Below are two of the most common techniques used in clinical practice:
Socket Preservation (Right After Extraction)
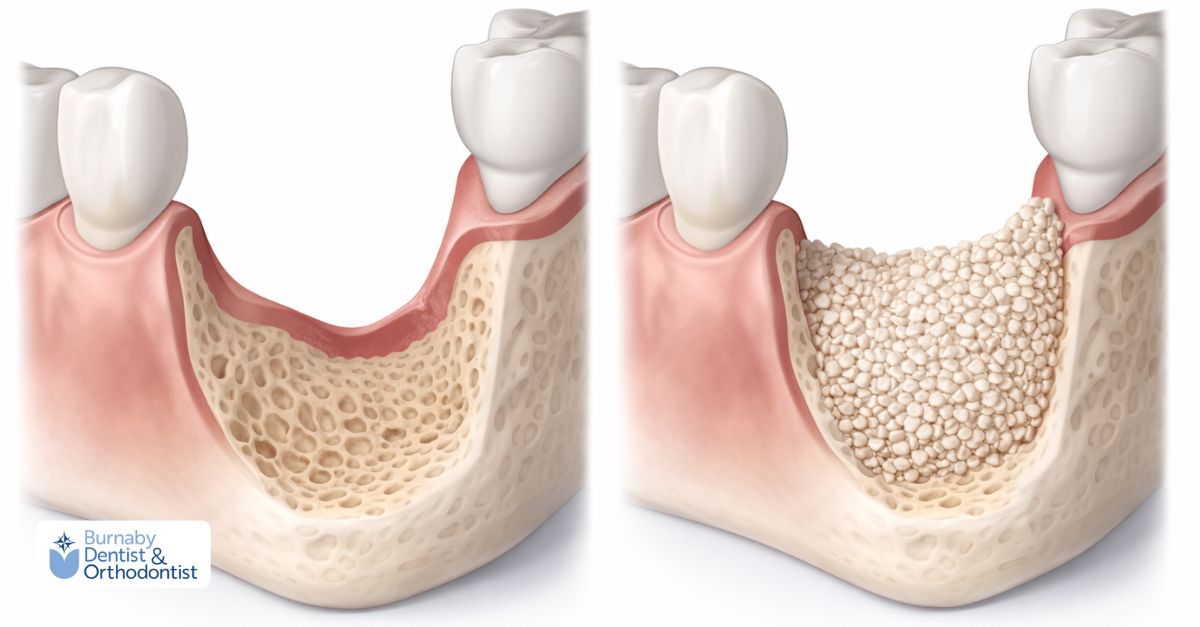
When a tooth is removed, the surrounding bone begins to shrink within weeks. Socket preservation prevents this loss by filling the empty space with graft material immediately after extraction.
This maintains the ridge’s height and width, ensuring your jawbone stays strong and ready for future restoration, especially dental implants for seniors.
By keeping bone volume intact, socket preservation also helps preserve your natural facial shape and reduces the need for more complex grafting later.
Sinus Lift (Upper Back Teeth)
In the upper molar region, the bone beneath the sinus cavity is often thin, making implant placement difficult. A sinus lift gently raises the sinus membrane and fills the space beneath it with bone graft material. Over time, this forms a solid foundation for stable implants.
It’s a common and predictable procedure, especially for patients who have been missing upper teeth for years or experienced bone resorption in the back jaw. The result is stronger bone support and improved implant success in the upper arch.
When Each Bone Graft Type Is Used
Each bone graft material serves a specific purpose depending on how much bone is missing and where it’s located. The table below highlights the most common clinical uses for each type.
| Graft Type | Typical Use |
| Autograft | Large defects or full reconstruction cases |
| Allograft / Xenograft | Ridge preservation or bone augmentation before implants |
| Alloplast | Small, localized bone repairs or minor contouring |
At Burnaby Dentist & Orthodontist, we tailor each grafting plan using CBCT imaging and digital 3D modeling to ensure optimal integration and long-term bone stability.
How Bone Grafting Works Biologically
Bone grafting doesn’t just fill a space. It helps your body rebuild bone over time. The healing process relies on three key biological mechanisms that work together to restore strength and volume.
- Osteoconduction: This is the foundation of most grafts. The material acts like a scaffold, giving your body a surface where new bone cells can attach and grow. It guides the shape and structure of new bone as it forms.
- Osteoinduction: In this stage, the graft releases natural proteins called growth factors. These signals tell nearby stem cells to transform into bone-forming cells, speeding up the healing and regeneration process.
- Osteogenesis: This happens only with grafts that include live bone-forming cells, like autografts. These cells begin building new bone tissue immediately, making the graft more active in the healing process.
Autografts support all three of these biological functions, which is why they’re often considered the most effective. Other graft types, like donor, animal, or synthetic materials, usually support osteoconduction and sometimes osteoinduction, but they don’t bring live cells to the site.
At Burnaby Dentist & Orthodontist, we carefully evaluate bone biology through digital 3D imaging before treatment to choose the graft that delivers the best long-term results for your smile.
Who Might Need Bone Grafting
Bone grafting can be recommended for several reasons, especially when jawbone loss affects your oral health or limits future treatment options.
Common Scenarios
Bone grafting is often used in the following cases:
- Post-Extraction: Preserves bone immediately after a tooth removal.
- Long-Missing Teeth: Prevents or reverses resorption where teeth have been absent for years.
- Periodontal Defects: Rebuilds bone lost to advanced gum disease.
- Trauma: Restores structure after accidents or surgical damage.
- Congenital Conditions: Addresses developmental defects, such as cleft areas, before implants or prosthetics.
Your dentist will use digital 3D imaging and CBCT scans to assess bone density and plan treatment precisely. Regular visits play a key role. Understanding why we should get a dental checkup helps you prevent issues that might later require bone grafting or implant surgery.
At Burnaby Dentist & Orthodontist, our dental technology allows us to capture detailed images of your jaw and design grafting plans that support both function and long-term stability.
What happens during a dental bone grafting procedure?
Dental bone grafting is usually performed as an outpatient procedure with local anaesthesia. The steps may vary depending on the graft location and material, but most treatments follow this general process:
1. Anaesthesia and Preparation: The area is numbed using local anaesthetic. Sedation may also be offered for patients who are anxious or undergoing a more involved procedure.
2. Incision and Cleaning: A small incision is made in the gum tissue to expose the area of bone loss. The site is then thoroughly cleaned and disinfected to prepare it for graft placement.
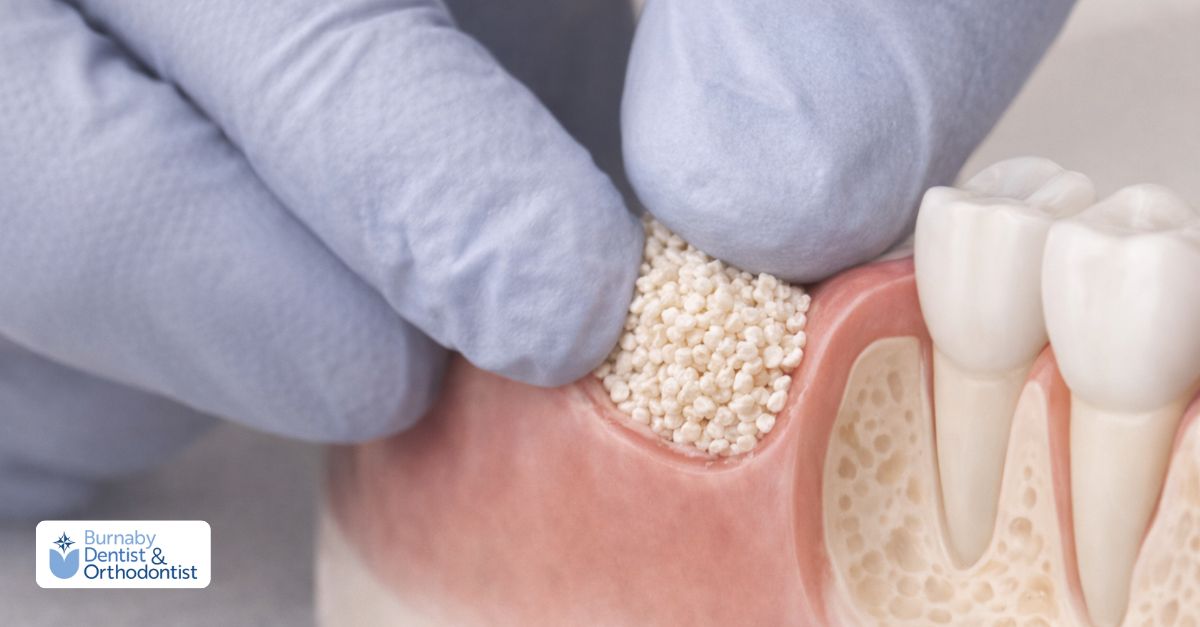
3. Graft Placement: The graft material is carefully inserted into the area of deficiency. Your dentist may shape it to fit the space precisely.
4. Membrane Placement: In many cases, a protective membrane is placed over the graft. This helps guide healing and keeps the graft material in place. Some membranes dissolve naturally; others may need to be removed at a later appointment.
5. Closure and Recovery: The gum tissue is repositioned over the graft and sutured closed. You’ll receive aftercare instructions and a follow-up plan to monitor healing and check graft stability.
Block vs Particulate: What You Might Hear Us Say
You may hear your dentist mention a “block” or “particulate” graft. Both refer to the form of material used.
Block grafts are solid bone sections typically used for larger defects, while particulate grafts are small granules ideal for filling smaller areas or sockets.
At Burnaby Dentist & Orthodontist, we select the format that best matches your bone anatomy and healing goals for stable, long-term results.
Healing and Aftercare Tips

Recovery after a dental bone graft is usually smooth, especially when you follow your dentist’s instructions carefully. While healing times vary depending on the size of the graft and your overall health, most patients return to normal routines within a few days.
Here are some tips to support healing and reduce discomfort:
- Manage Swelling: Apply ice packs to the outside of your cheek in the first 24–48 hours. This helps reduce swelling and bruising. Use 15-minute intervals on and off.
- Control Bleeding: If slight bleeding occurs, apply gentle pressure with a gauze pad. Avoid rinsing aggressively or touching the area with your tongue.
- Take Prescribed Medications: Follow all instructions for antibiotics or pain relievers. Don’t skip doses, even if discomfort seems minimal, as this prevents infection and controls inflammation.
- Eat Soft Foods: Stick to soft, cool or lukewarm foods for the first few days. Avoid anything hard, crunchy, spicy, or hot that could disturb the graft. Sticking to a soft food diet is key after surgery, and guidelines such as what to eat after gum grafting also apply to bone grafting recovery.
- Maintain Oral Hygiene: Keep your mouth clean, but be gentle around the surgical site. Your dentist may recommend a medicated rinse. Avoid brushing directly over the graft until told otherwise.
- Attend Follow-Ups: Your dentist will schedule follow-up visits to monitor healing and ensure the graft is integrating properly. Don’t miss these appointments—they’re essential to long-term success.
Most patients experience only mild swelling and discomfort for a few days. Serious complications are rare but should be reported immediately.
Following these aftercare tips not only supports graft integration but also helps you Heal Faster After Extraction, reducing discomfort and improving recovery time.
Recovery Timeline (Typical)
Healing happens gradually as your bone graft integrates with natural tissue. The outline below shows what most patients can expect at each stage.
| Phase | Typical Progress |
| Day 1–3 | Swelling, Ice Packs, Soft-Food Diet |
| Week 1–2 | Suture Check, Gentle Hygiene Resumed |
| Week 3–6 | Discomfort Subsides, Normal Diet Gradually Returns |
| Week 6–12 | Bone Integration Actively Underway |
| Month 3–6 | Implant Evaluation or Follow-Up Imaging (Case-Dependent) |
Benefits of Bone Grafting
A well-executed bone graft doesn’t just restore missing tissue—it lays the foundation for future dental health and long-term function. Whether you’re planning for implants or preventing bone loss after an extraction, grafting offers several important benefits.
- Improved Function: Bone grafting restores jaw strength and volume, enabling comfortable chewing and clear speech while supporting stable implant placement.
- Enhanced Facial Appearance: Loss of bone volume can make the face look sunken. A bone graft helps maintain natural contours by rebuilding the jaw’s structure.
- Better Oral Health: By stabilizing the bone around nearby teeth, grafting prevents further bone deterioration and protects against shifting teeth, gum recession, and long-term bite changes.
- Predictable Treatment Outcomes: Grafting increases the success of restorative procedures, especially dental implants, by ensuring there is sufficient healthy bone support, making your treatment plan more reliable.
Risks and Considerations
While dental bone grafting is generally safe and effective, it’s still a surgical procedure, and like any surgery, it comes with some potential risks.
- Surgical Site Discomfort: Autografts, which use bone from another part of your body, may cause additional soreness at the donor site. This is temporary but may extend recovery slightly.
- Infection or Bleeding: Infections are rare but possible. Some minor bleeding is expected after surgery, but prolonged or heavy bleeding should be reported to your dentist right away.
- Nerve Irritation: If the graft site is close to nerves, especially in the lower jaw, there’s a small chance of temporary numbness or tingling in the lips, chin, or tongue.
- Graft Rejection or Failure: Sometimes the graft doesn’t fully integrate with your natural bone. This could be due to smoking, poor oral hygiene, or systemic health issues. In such cases, a second procedure may be needed.
Discuss any medical conditions, medications, or concerns with your dentist in advance. Careful planning helps reduce risks and supports a smoother recovery.
We’ll review medications and systemic conditions, such as diabetes, smoking, or autoimmune issues, because they can influence healing and graft success.
How long does recovery take?

Healing after a dental bone graft happens in two main phases: short-term recovery and long-term integration.
Most patients feel better within a week. Swelling, tenderness, and minor discomfort usually improve during this time, allowing you to return to soft foods and light activities.
However, the bone graft itself takes longer to fully heal. In most cases, your body needs at least three months to integrate the new material. For larger or more complex grafts, full healing may take up to nine to twelve months.
Your dentist will monitor your progress through follow-up appointments and imaging to determine when you’re ready for the next step, such as implant placement or further treatment.
At Burnaby Dentist & Orthodontist, we combine digital 3D imaging and precise planning to prepare your jaw for long-term restorations, including dental implants in Burnaby.
Final Thoughts
Bone grafting plays a vital role in rebuilding lost jawbone, supporting implants, and preserving facial structure. Though it involves patience during healing, the benefits of stronger bone, improved function, and a more confident smile make it a worthwhile investment in long-term oral health.
Not sure if you need a graft? Book a quick imaging visit in Burnaby and leave with a clear, personalized treatment plan.
If you’re weighing your restoration choices, our team can also explain the difference between an implant vs dental bridge to help you plan confidently.
At Burnaby Dentist & Orthodontist, we combine digital 3D imaging and comprehensive diagnostics to assess bone health and guide every step of your care. Whether you need grafting, implants, or preventive treatment, our team ensures your foundation is healthy, stable, and ready for the next phase of your smile.
Book your consultation today to explore personalized dental care and advanced bone grafting options in Burnaby.
Is bone grafting always required before getting implants?

Not always. If you have enough bone to support an implant, grafting may not be necessary. Your dentist will confirm this with imaging and clinical exams.
Will the procedure be painful?

Bone grafting is usually done with local anaesthesia or sedation. Most patients report mild discomfort after the procedure, which is manageable with medication.
What materials are used in a dental bone graft?

Grafts can be made from your own bone (autograft), donor tissue (allograft), animal bone (xenograft), or synthetic material (alloplast). Your dentist will choose the best option based on your needs.
Can a bone graft fail?

Failure is uncommon but possible. Risks include infection, rejection, or lack of integration. Good oral hygiene, not smoking, and attending follow-up visits improve the chances of success.
How soon after extraction should socket preservation be done?

Ideally, at the same appointment as the extraction, to protect the ridge shape and maintain strong bone for future implant placement.